Enhancing Your Vision
Guiding you toward the procedure that fits your unique needs, so you can see the world clearly and confidently.
24
Nov
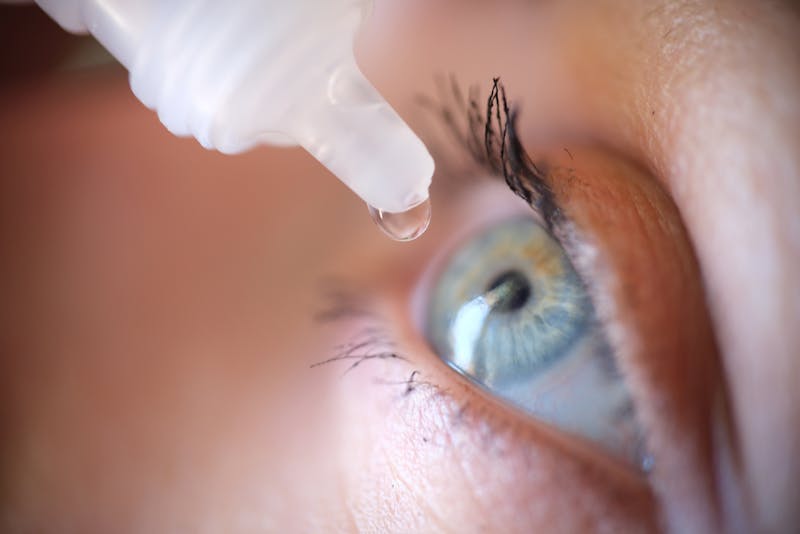
Many people think cataract surgery is over once the cloudy lens is removed. But the truth is, what happens after surgery often determines how clearly you'll see for the rest of your life. Surprisingly, it can all go wrong because of one small bottle, the anti-inflammatory e...
29
Oct

You've been told to wait for the “perfect” 2026 cataract lens. But what if waiting means worse vision or fewer options? In my Manhattan and New York City practice, many patients ask exactly that question. If you’re considering cataract surgery or lens repl...
14
Oct

Thinking about cataract surgery, or already had it? Most people enjoy crisp, glasses-free vision. Yet a real fear lingers: What if I end up with glare, halos, or blur that glasses can't fix? The good news: for many patients, there’s a straightforward, predictable way ...
06
Aug
Cataract surgery in New York City has come a long way. Once seen as a standard procedure with a basic outcome, cataract surgery today is more advanced, more customizable, and more life-changing than ever before ; especially in a world-class setting like Manhattan. If you're consi...
06
Aug

Dry eyes affect millions of people worldwide, and if you've been frustrated by treatments that haven’t worked, you’re certainly not alone. A common reason for treatment failure is inaccurate diagnosis or a lack of specialized knowledge about dry eyes. In this ar...
06
Aug
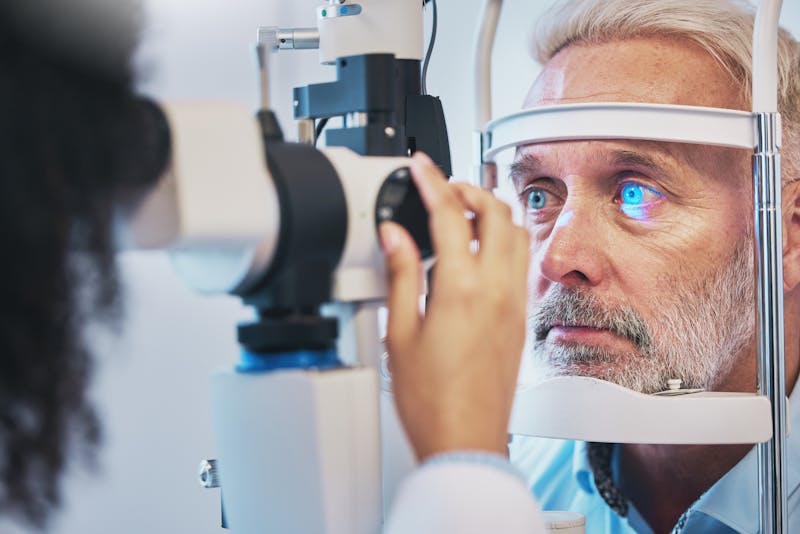
Are you finding it harder to read or noticing things look blurrier up close? If so, you're not alone. After the age of 40, many people experience difficulty focusing on near objects, a condition known as presbyopia. As a result, you may need to update your glasses prescript...
06
Aug

Are you suffering from dry eyes and haven't found relief with existing treatments? You're not alone—dry eyes impact nearly 20% of the U. S. population and cost over $55 billion annually in healthcare and lost productivity. But here’s some exciting news: new appro...
11
Jun
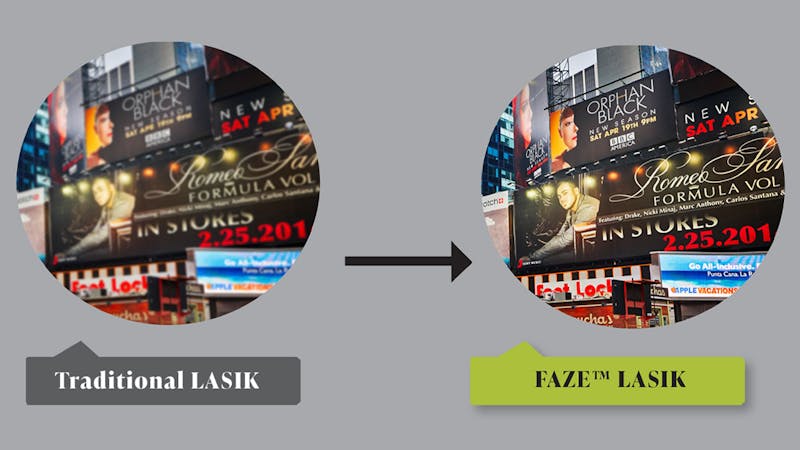
Beyond Traditional LASIK: Discovering the Hidden Key to Perfect Vision Are you thinking about getting LASIK? Or maybe you've already had the procedure but still struggle with less-than-perfect vision? What if there's an innovative technique designed to overcome the limitati...
11
Jun
Key Takeaways Lens choice defines your vision: Your lens implant is permanent and impacts how you see daily, with 2025 options offering advancements like glare-free night vision and eliminating the need for glasses. Popular 2025 lens options: Choices like Puresee for glare-f...
11
Jun
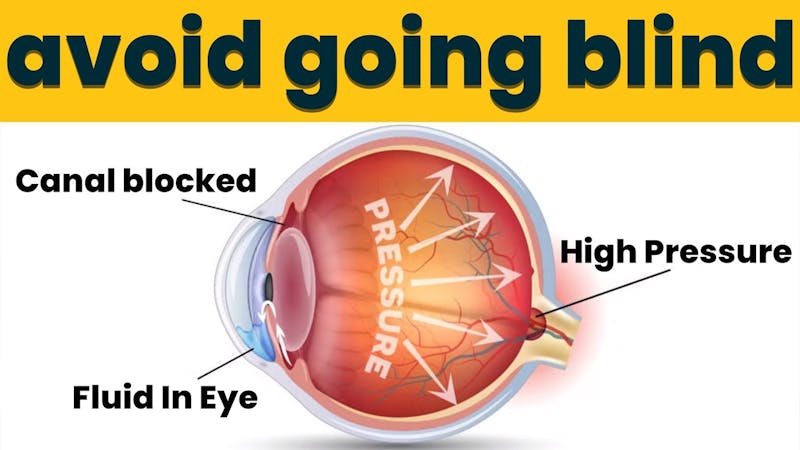
Prevent Glaucoma Glaucoma, often referred to as the “silent thief of sight,” is a condition that affects millions of people worldwide. It's a leading cause of irreversible blindness, and the most concerning part is that it often develops without noticeable sympt...
11
Jun

Key Takeaways Pick a dedicated specialist: Look for a surgeon who focuses solely on surgery rather than general eye care. Expertise with premium lenses: Choose a surgeon experienced with lenses that correct astigmatism and presbyopia. Ask the right questions: Consider their ...
11
Jun

Key Takeaways Presbyopia is an age-related vision change that starts around age 40 due to the eye's lens losing flexibility. Common myths include confusing presbyopia with farsightedness and thinking it can be cured with LASIK or glasses. Treatment options range from reading g...
Guiding you toward the procedure that fits your unique needs, so you can see the world clearly and confidently.




If you do not see your preferred date and time please call the office, so we can accommodate your request (917) 398-4011.